Why I Stopped Eating Meat, Then Started Again After Ten Years
Plants are full of iron, but they won’t let you have it
Image
I gave up eating meat in the early 90s. I didn’t mean to: my original intention was to forgo meat from factory-farmed animals and eat only organically-reared, free-range produce. The problem was, I couldn’t find any.
I knew of one butcher’s whose products met my high-minded spec, but getting there involved a cross-London schlep that quickly proved impractical. It was easier, and considerably cheaper, to stop eating meat altogether.
This decision was motivated by a resolve to disassociate myself from the horrific and inhumane practice of intensive livestock farming. Thus began my one-woman boycott, a small and, quite frankly, insignificant stand.
For around 10 years or so I ate a mainly vegetarian diet supplemented with fish and seafood two or three times a week. These days you’d call it a flexitarian diet. At the time I had no idea I was so on-trend, ahead of my time.
My culinary repertoire was constructed on various layers of wholegrains (plenty of brown rice) and tofu (a curious blend of the punitive and the bland). I was a nutritionist, so felt duty-bound to strive for certain standards (or rather delusions), such as wholemeal pasta - an abomination with as much flavour and appeal as workhouse gruel.
Some foods were quite passable. Beans and lentils, for example, which lend themselves well to any number of creative combinations. I ate organic, free range eggs and dairy foods. I couldn’t contemplate a life without cheese and all its glorious incarnations.
Being a nutritionist, I understood the importance of ensuring adequate intake of all the essential nutrients. I made a point of including a generous serving of steamed leafy greens with each main meal, to provide iron. I considered iron to be the weak link in my diet plan.
Kale, spinach, broccoli, cabbage… I ate them all. They do indeed contain very respectable levels of iron. Plus, they are loaded with vitamin C, a nutrient that enhances iron absorption. As part of my belt-and-braces approach I also took a daily vitamin C supplement. I didn’t drink tea or coffee at the time, which was to my advantage as both can inhibit iron absorption.
I had every angle covered. I was practising what I had been taught — and of course, I was a nutritionist!
Iron in the blood… or not
Ten years later, and I am in the basement laboratory of the university building in London where I am a lecturer. A group of us are keeping ourselves entertained by taking various blood tests. I opt for an iron test.
My iron levels are dangerously low. It’s a miracle that I am still upright, and mobile.
The shock of this revelation makes me think. I knew I had symptoms that possibly signified iron deficiency — fatigue, light headedness, pallor — but until now had successfully managed my denial.
In creeps the thought of eating meat again. Once it has put down roots, I relish the idea, which has suddenly taken on an urgent medicinal quality. I need meat. And times have changed: meat from free-range, organically reared animals is now readily available for purchase without having to make travel arrangements.
I start with sausages (easy to cook), and soon fall upon the whole fleshy smorgasbord with a renewed and voracious appetite.
I quickly feel a whole lot better, sensing my iron levels rising like sap in spring. This instinct is confirmed by a blood test a few months later. Normal iron has been resumed.
The irony
So why weren’t those interminable leafy greens and beans enough?
When it comes to nutrients in food, eating and absorbing are two very different matters, the former being much easier to accomplish than the latter.
And therein lies the nub. There is plenty of iron in plant foods, but it has very low bioavailability, meaning that instead of being absorbed, most of it sails straight through you on a sea of peristaltic waves. Your blood is not the final destination of this ship.
There are two forms of dietary iron: haem and non-haem. Haem iron has high bioavailability and is unique to animal-source foods, which also contain non-haem iron. Plant foods contain non-haem iron, but no haem iron.
The human gut can absorb 25% — 30% of haem iron from animal-source foods. That’s quite a good return: giving back is part of the circular nature of nourishment.
When it comes to non-haem iron from plant sources, you give much more than you take. Non-haem iron absorption can be as low as 2%.
Blame it on the phytate
Those plant foods that I consumed with such gusto may be full of worthy nutrients, but they are also full of anti-nutrients. These unsporting chemicals act as iron inhibitors. The most potent of all is phytate, and its effect is dose dependent. The more you consume, the less iron you absorb.
Phytate is a compound found in high amount in grains (especially those ‘healthy’ wholegrains) seeds, nuts and beans. Phytate forms complexes that bind not only to iron but also zinc and calcium. Because humans lack phytase, the enzyme that breaks down phytate, minerals pass largely unabsorbed through the body. There is however, no phytate in animal-source foods.
Because phytate is heat stable, it is not easily degraded by cooking. And although other processing methods such as soaking can reduce the phytate content to some extent, this effect is … “unlikely to be sufficient to overcome the shortfalls in iron, zinc, and calcium that have been consistently reported in cereal-and/or legume-based complementary foods.”
Like wholegrains, beans have high levels of phytate, but soya beans go the extra mile. My regular tofu consumption wasn’t just joyless, it was doing nothing for my iron status. That’s because the protein in soya beans has an additional iron-blocking effect, independent of the phytate content.
You can improve iron absorption from plant sources by consuming vitamin C-rich foods with your meal. Vitamin C is known to enhance uptake of non-haem iron, but — as confirmed by personal experience — it is considered unlikely to counteract the effect of iron inhibitors, such as phytate, and another one — polyphenols. Polyphenols are found in varying amounts in vegetables, fruit, cereals, beans, tea, coffee and red wine.
Who’s who in the world of iron deficiency
I was iron deficient, yet neither malnourished nor impoverished. In other parts of the world, where malnutrition and poverty co-exist, low blood iron is a virtual given.
According to the World Health Organization, iron deficiency is the most common global nutritional deficiency, and the main cause of anaemia. Anaemia affects around a third of the world’s population - mainly infants, women of childbearing age and pregnant women.
Whereas iron deficiency is common in developing countries, and its root cause is poverty, people in industrialized countries are more likely to experience deficiency for the same reason I did: consciously excluding the most bioavailable source of this mineral from the diet.
Iron status in vegetarians is often low, despite an iron intake that is comparable to that of omnivores.
This observation was confirmed by a review of published data on the iron status of vegetarian adults, compared to non-vegetarian adults. The results of thirteen studies that examined the blood (serum) ferritin levels of vegetarians in Australia, Canada, China, England, Germany, Korea, New Zealand, South Africa and the United States were pooled, and the authors of the study concluded that:
“The findings based on ferritin levels showed a high prevalence of iron depletion among vegetarian participants, especially among females.”
“The prevalence of low ferritin was higher among both vegetarian males and females, compared to their nonvegetarian counterparts”
“Thus, iron is rightly considered a nutrient of concern for vegetarians. This is especially true for premenopausal vegetarian women.”
Although vegetarian diets may contain the same level of iron as meat-based diets, the poor absorption rate of non-haem iron means that vegetarians may need to increase dietary iron, according to one calculation, by 80%.
Over the last few years, my interest in the role and biochemistry of iron has taken a new direction, with my ongoing research into brain nutrition. Iron is normally associated with blood, oxygen and energy, and its role in brain function often takes a back seat. I have been researching and writing a book on diet and cognitive function and have been struck by just how critical iron is to the development of intellect.
As an adult, my own deficiency status was easy enough to rectify through diet. The population group that should concern us most are babies and children.
Iron deficiency is a particular problem for children, as it reduces intellectual performance and leads to cognitive defects. Iron deficiency is particularly common during pregnancy, a situation that is associated with delayed cognitive development.
If there is iron deficiency in early life, there is also greater risk of developing psychiatric problems as older children. Iron deficiency anaemia is: “probably related to childhood/adolescence-onset psychiatric disorders.” These disorders include mood disturbances, ADHD and autism. Iron deficiency anaemia has been identified in up to 30% of children with autism spectrum disorder.
If you are concerned about your own iron status, I strongly recommend a blood test to determine this. You may need to take iron supplements, but only on the advice of your physician, because some people suffer from an iron-related condition called hemochromatosis, and iron is the last thing they need.
Hemochromatosis arises when too much iron accumulates in the body. Humans have no mechanism to excrete excessive iron, and ordinarily only absorb what is needed from food. In hemochromatosis, the body absorbs too much iron and has to store the surplus in joints and organs — the liver, heart and pancreas are usually affected.
Hemochromatosis is uncommon, and almost always hereditary — a mutation in a gene that is passed from parents to child — but can be caused by non-genetic factors, such as liver disease. You are much likely to be affected if you are of Northern European descent. National statistics are few, but we do know that hemochromatosis affects around 1 in 300 Canadians.
How much?
This is the daily amount of iron recommended in the UK and the US.
As I said above, consuming that much iron isn’t a problem. It’s absorbing that much. Iron has to get from gut to blood, and if that doesn’t happen, it has no nutritional value.
Don’t depend too much on processed foods that have been fortified with iron. Many cereal foods are fortified with “low-cost elemental iron powders” that are not recommended by the World Health Organization and have very low bioavailability.
These days I eat a lot of meat, and fish. I buy, whenever possible, pasture-fed meat, an evolutionary step that is above and beyond organic produce. Animals that are pasture-fed live outdoors almost all-year round. Pasture is not just about grass — it’s the full natural diet of these herbivores and includes wild flowers, clover and herbs.
Pasture-fed animals are never given soya, or cereals, or any other manufactured feed, as these do not form part of their natural diet. Welfare standards are high. So too is iron, and iron bioavailability.
No hair shirt regimen required.





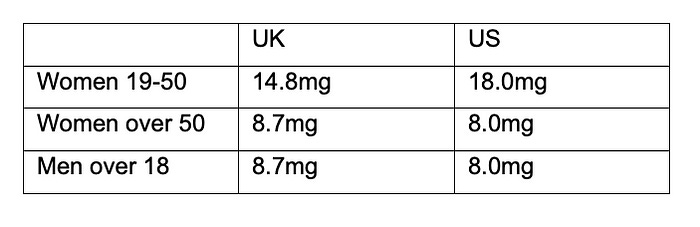
The variations in recommendations are due entirely to the fact that they are just estimates. Between you and me, nobody really has a clue how much we should consume of any one nutrient. But I wouldn't recommend attempting to get anything from wholemeal pasta, or gruel.
I love a nicely turned phrase, and this one is a gem: "... an abomination with as much flavour and appeal as workhouse gruel". I've never had gruel, nor have I lived in a workhouse, though as a teenager I sometimes believed I was living in one. Moving on, I noticed that recommended daily iron numbers were different in UK from those in the US. Is this just due to differences of opinion in those who set the numbers, or are there environmental differences that affect the values? Given the abysmal state of US food, I'd have expected the values to be reversed.